Dupuytren's disease
What is it?
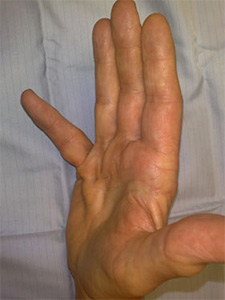
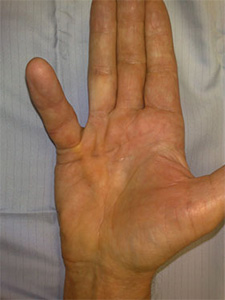
Baron Guillaume Dupuytren, a French Surgeon, first described Dupuytren’s disease in 1831. In this common condition there is over growth of certain cells under the skin of the palm. It initially starts as firm lumps which appear just below the skin. These nodules can be tender in the early stages and form small pits. They gradually progress to form cords that prevent the finger straightening completely and the digit is gradually drawn in towards the palm. Nodules can form over the top of the finger knuckles (Garrod's knuckle pads). In some people such nodules or cords may develop on the soles of the feet.
Is it called by any other name?
Dupuytren’s contracture.
What is the cause?
The condition usually arises in middle age. It is more common in men. The cause is unknown, but it is more common in Northern Europe and often runs in families. It is believed that the Vikings brought the disease into Great Britain. It is usually present in both hands and may be associated with diabetes, smoking, high alcohol consumption, chronic lung disease and epileptic medication. The majority of patients have none of these medical conditions. It can also occur after an injury to the hand or wrist. It is not associated with manual work. The ring and little fingers are usually involved.
What are the symptoms and how is the condition diagnosed?
Patients present at varying stages of the disease. Generally the condition is noticed because of the inability to place the hand flat on an even surface. Dupuytren's disease begins with a small lump or a series of lumps in the palm. The lumps are usually stuck to the skin and can be tender in the early stages but the condition is nearly always painless. In about a third of patients these nodules gradually extend over months and form a cord. The cord pulls the finger into the palm causing a contracture. If left alone the finger becomes fixed. The disease also affects the web spaces and the hand span becomes reduced. The earlier the age at onset the more severe the disease will be.
Will further tests or investigations be needed?
The diagnosis of a Dupuytren’s disease is made clinically and no special investigations are needed.
What is the treatment?
There is no cure for the condition. Surgery is the only treatment that will make bent fingers straighter, but it may not be possible to always make them fully straight. Surgery will not eradicate the disease. While most patients need only one operation it is possible that Dupuytren's disease may reappear after an operation either at the same site or another area of the hand.
Depending on the extent of the disease and disability, the surgeon can recommend the timing and type of surgery. If surgery is planned it can be carried out under local, regional or general anaesthetic. In a vast majority of patients the procedure is done as a day case.
The various surgical options are:
Percutaneous Fasciotomy or Needle Aponeurotomy. In certain patterns of contracture it is possible to weaken and then release the cord that is causing the contracture percutaneously with a needle. It is most effective for disease in the palm of the hand and with well-defined cords. Recurrence of contracture is high after this surgery but it will be some time before the patient needs further surgery.
Fasciectomy. This type of surgery is most commonly practised and it involves excising the entire cord(s). The incision is closed in a zigzag shape to prevent contracture due to scars.
Dermofasciectomy. This type of surgery is reserved for aggressive cases or for recurrence of the disease. Here, the Dupuytren’s tissue is removed together with the overlying skin. The area is then replaced with a skin graft usually taken from the forearm. This is a more complicated operation and it takes longer to recover.
Amputation. In rare, neglected, un-operated cases, or when the disease has recurred many times resulting in a severe contracture, amputation of the finger may have to be considered.
The therapy and splinting after surgery will depend on the extent of the contracture and the type of surgery performed. Generally the hand is splinted in a plaster splint for a few days to keep the fingers straight immediately after surgery; the arm needs to be elevated to reduce swelling and a hand therapist will aid with rehabilitation. The wound is checked within a few days and a thermoplastic splint is made. The splint is worn regularly for the initial 2-4 weeks and then at night for between 6-12 weeks after surgery. The stitches are removed within 10-12 days. If a skin graft has been used the graft may be sewed in over a sponge dressing, which needs to be maintained for two weeks.
What happens if it is not treated?
It is not possible to predict the progression of the disease. In about half the patients the disease will progress and cause a finger contracture. As the finger bends it will cause secondary stiffness in the finger joints.
What is the success of surgical treatment?
The success of surgical treatment is variable with regards to the degree of improvement achieved. The final outcome is dependent on many factors including the extent and behaviour of the disease itself, the duration since onset, the extent of pre-operative contracture and the type of surgery required. It is not always possible to make the fingers fully straight. Generally the longer the duration of deformity, the lower the chances of achieving full correction.
Contractures that only affect the MCP joint (large knuckles that you see on the back of your hand) are most predictably helped by surgery. Contractures that only affect the PIP joint (knuckles in the middle of the finger) are most likely to recur after treatment. Most contractures are combined and some of them will also involve the DIP joint (end joint of the finger).
What are the complications of surgical treatment?
Incomplete correction (especially in severe and long standing deformities).
Delayed wound healing. Portions of the skin especially at the tip of the zigzag scar may be slow or fail to heal. This is especially of concern in patients who smoke or have diabetes.
Infection of the wound is possible but can usually be successfully treated.
Recurrence of disease and contracture (One in three chance recurrence at five years).
Digital nerve damage. The nerves that run on either side of the finger could be potentially damaged at surgery. If this happens the nerve is immediately repaired but permanent numbness may follow.
If a skin graft has been used it may fail to incorporate.
Severe complex regional pain syndrome (CRPS) is a rare but serious complication after hand surgery. Unfortunately it is not possible to predict this problem but it needs to be monitored and treated (usually with physiotherapy) if it develops.
Any surgical intervention has the risk of developing complications, which are unpredicted. These complications may have the potential to leave the patient worse than before surgery.
Is there anything I can do to improve outcome?
After surgery keep the hand up so as to help reduce swelling. I would advise against wearing rings on the operated hand for 6 weeks following surgery. Start exercising your fingers immediately after surgery. This will help to avoid finger swelling and stiffness.
Keep the wound dry. Once the stitches have come out the scar can be massaged regularly with a soft, non-perfumed cream for a couple of months. If the scar is tender to press, tapping along the scar and on either side of it firmly with your fingertips a few times a day may be useful. Also try to become used to putting pressure through your hand and wrist again. It is quite normal for this to feel uncomfortable at first.
When can I do various activities?
This depends on the extent of the contracture, the extent of surgery needed and your occupation. Generally patients may be able to return to a simple desk job within 3-4 weeks of surgery, but heavy manual work should be avoided for about 6 weeks. Driving should be possible within 3-4 weeks of the operation. This will also depend on the side operated and the type of car to be driven i.e. manual or automatic


 MENU
MENU