Carpal Tunnel Syndrome
What is it?
The hand is supplied by three nerves. One of them is called the median nerve and like a telephone cable it passes through a protective conduit (a tunnel) on the front of the wrist. This tunnel is called the carpal tunnel. It also contains tendons that bend the finger and thumb. The nerve can get compressed in this tunnel and cause symptoms. The condition is known as a Carpal Tunnel Syndrome.
What is the cause?
This is a very common condition and in the majority of patients we do not know what causes this syndrome. It usually occurs in middle age and women are prone. The condition is also associated with pregnancy, thyroid problems, diabetes, previous wrist fractures, arthritis and rheumatoid disease.
What are the symptoms and how is the condition diagnosed?
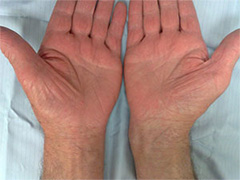
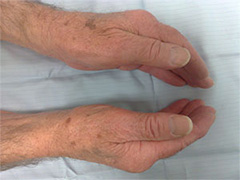
The main symptom is tingling or pins & needles in the hand. The symptoms usually affect the thumb, index, middle and ring fingers. This is because the median nerve supplies these fingers. Tingling is often worse at night or first thing in the morning. It may be provoked by gripping. In the early stages the symptoms are intermittent but later become continuous as the condition worsens. The patient will notice numbness in the fingers and thumb together with weakness and wasting of the muscles at the base of the thumb (See picture). They may drop objects and feel clumsy with their hand(s). They may also complain of pain in the wrist and forearm.
Will further tests or investigations be needed?
The diagnosis of carpal tunnel is made clinically but you may be referred for electrical tests (nerve conduction studies). These may be to confirm the diagnosis in patients in whom the symptoms and signs are not classical.
Some patients have what is called a 'double crush syndrome' in which the median nerve also may be compressed elsewhere (usually in the neck from where it begins).
What is the treatment?
Splints may be useful if worn at night or with activities that aggravate the symptoms. A local injection of steroid may relieve symptoms. The injection very occasionally causes some thinning or colour change of the skin at the site. Improvement is variable and can be temporary. A potential risk of such an injection is damage to the median nerve itself.
The standard operation advised is an open surgical release of the carpal tunnel. A skin incision of 3-4 cm is required (see picture) and at surgery the roof of the carpal tunnel is opened thereby decompressing the median nerve. The procedure is usually carried out under local anaesthesia as a day case. At surgery a tourniquet cuff is applied around the forearm so as to stop bleeding and make the operation safer and quicker. This tourniquet is needed for about 10 minutes and can be uncomfortable in a small number of patients.
After the operation a sticky dressing is applied over the surgical wound. A bulky supportive cotton-wool dressing is then applied. This supportive dressing is reduced after a couple of days. The small sticky dressing should be left for 10 -12 days when the stitches will need to come out. The arm should be kept elevated after surgery for 1-2 days as this will prevent the fingers from swelling and causing discomfort. Light use of the hand should be possible from the day of surgery. Active movements of the finger are recommended soon after surgery.
Some surgeons advise endoscopic decompression of the carpal tunnel (keyhole surgery). A telescope is used and surgery is visualized on a monitor. A smaller incision is needed and an earlier return to work is possible. The risks associated with the procedure are greater. It is debatable as to whether the benefits of this procedure significantly outweigh the risks.
When the syndrome is associated with certain other conditions like rheumatoid arthritis, clearing of the soft tissue lining of the tendons (synovectomy) may be required.
What happens if it is not treated?
Some mild cases of carpal tunnel syndrome may recover spontaneously. If the condition occurs during pregnancy it may resolve after the baby is born. If the condition is neglected most people will find that their symptoms will get progressively worse. The median nerve will continue to be compressed resulting in total, constant numbness, wasting and weakness of the muscles supplied by the nerve in the hand. This will lead to permanent, irreversible muscle weakness affecting function.
What is the success of surgical treatment?
The operation has a 90% success rate. It results in good resolution of night pain and pins / needles within a few days. Grip strength should come back to normal within a few weeks. However if the condition has been present for a long time, then recovery from symptoms such as constant numbness and muscle weakness is unpredictable.
What are the complications of surgical treatment?
The surgical scar may appear reddish for 2-3 weeks and may be tender for 6-8 weeks. However it is seldom troublesome in the longer term. Some patients may notice pain and tenderness on either side of the scar for 2-3 months. This is caused anterior pillar pain and is due to the released ligament (roof of the tunnel).
Infection of the wound is possible and in the early stage can be successfully treated with antibiotics. If pain increases after surgery, infection needs to be ruled out.
Stiffness of the finger joints is possible and hence the need to exercise them soon after surgery.
Severe complex regional pain syndrome (CRPS) is a rare but serious complication after hand surgery. Unfortunately it is not possible to predict this problem but it needs to be monitored and treated (usually with physiotherapy) if it develops.
Damage to the median nerve is possible but very rare when the open surgical technique is used. The risk is higher when the endoscopic technique is used.
Any surgical intervention has the risk of developing complications / setbacks which are unpredicted. These complications may have the potential to leave the patient worse than before surgery.
Is there anything I can do to improve outcome?
After surgery keep the hand up so as to help reduce swelling. I would advise against wearing rings on the operated hand for 4-6 weeks following surgery. Start exercising your fingers immediately after surgery (make a fist, and then stretch your fingers out; bend your wrist forwards and backwards and touch each finger tip in turn with your thumb). This will help avoid finger swelling and stiffness.
Keep the wound dry. Once the stitches are removed the scar can be massaged regularly with a soft, non-perfumed cream for a couple of months. If the scar is tender to press, tapping along the scar and on either side of it firmly with your fingertips a few times a day may be useful. Also try to become used to putting pressure through your hand and wrist again. It is quite normal for this to feel uncomfortable at first.
When can I do various activities?
Return to work depends on many factors including the nature of the job and hand dominance. Generally patients can return to a desk job within a few days and perform reasonable tasks with the hand. Avoid pressing heavily on the scar. Manual work should be avoided for 4-6 weeks. Driving should be possible within a week of the operation.


 MENU
MENU